Recent
Iceberg Product Management
·511 words·3 mins
Why I Schedule 25-Minute Meetings
·497 words·3 mins
AMSA - 1990
·10 words·1 min
No Margin, No Mission
·1572 words·8 mins
VLAN Through SpeedFusion
·1564 words·8 mins

Hydrow Drag Repair
·1399 words·7 mins
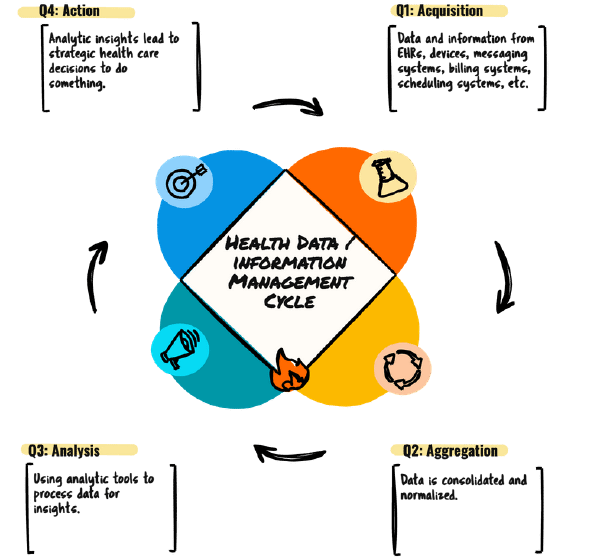
AAAA (the four A)
·862 words·5 mins
4 Key Strategies for Impactful Presentations
·549 words·3 mins

Pledges
·1727 words·9 mins
How Guinness Invented the t-Test for Health Research
·676 words·4 mins
ONC Turns 20!
·537 words·3 mins
NYHER RFA - Addendum #3
·204 words·1 min

FHIR and SCNs - NY 1115 waiver
·22 words·1 min

Social Care Networks - NY
·464 words·3 mins
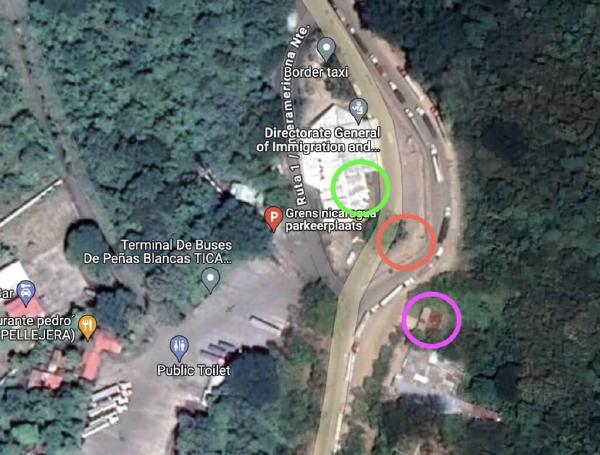
Health > Care, Border Runs
·1725 words·9 mins
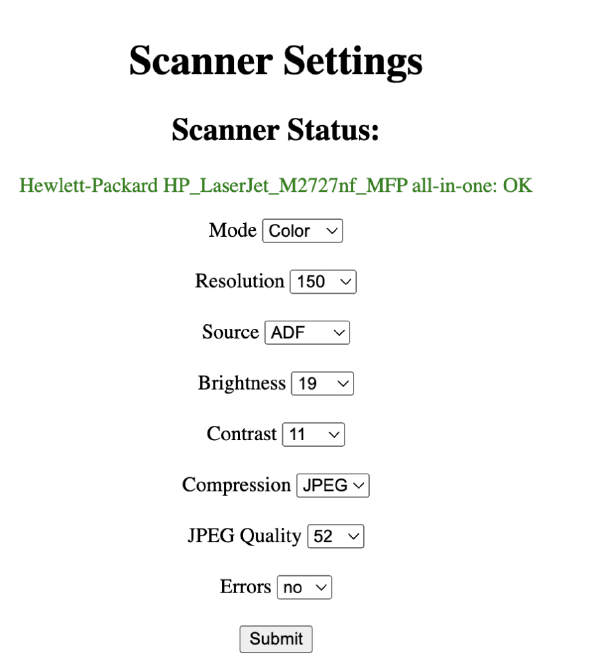
ChatGPT Builds a Scan Server
·503 words·3 mins

Pulling The Rope
·121 words·1 min
Welcome Back Kotter: New York's next 1115 Waiver
·7530 words·36 mins

Primary Health! Now from Circulo
·988 words·5 mins
Organizational Optimization
·828 words·4 mins